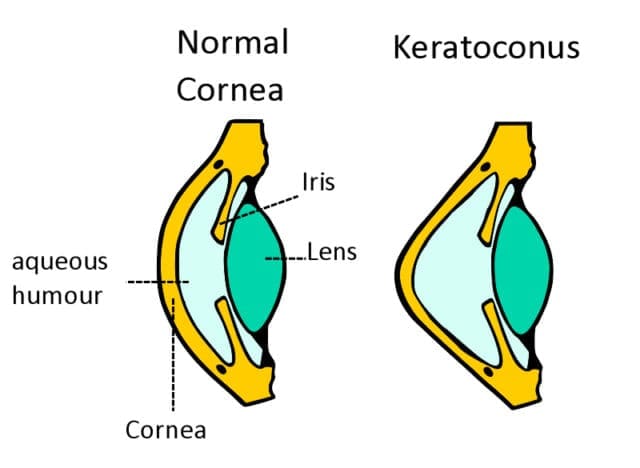
Keratoconus occurs when the cornea thins and slowly bulges outward to form a cone shape. The cornea is originally clear and dome-shaped and is located on the front surface of the eye. However, the cone-shaped cornea leads to blurred vision and may also cause the eye to be sensitive to light and glare. This eye problem often affects both eyes, although one eye is more commonly affected than the other. It also typically begins to affect people when they reach the ages of 10 and 25.
Moreover, the condition may progress slowly for a decade or longer. Therefore, it is recommended to go for regular eye checkups to help detect and treat eye diseases in their early stages. You can find local eye doctors for a comprehensive eye exam.
Signs
The condition’s signs and symptoms help identify the disease and its progression, although this may change over time. Regardless, the signs to watch out for include distorted or blurred vision, a frequent need to change eye eyeglass prescription, clouding vision, sudden worsening of vision, and increased sensitivity to glare and bright light, which can be problematic when driving at night.
Complications are also likely to develop if you have keratoconus. In some cases, the cornea may swell rapidly, resulting in sudden reduced vision and even cause the cornea to scar. This may be caused by a condition whereby the cornea’s inside lining breaks down, causing fluid access to the cornea. In most situations, the swelling subsides by itself without needing treatment, but a scar may develop and affect your vision. When the condition advances, the cornea may also begin to become scarred, especially where the cone seems most prominent. With a scarred cornea, your vision problems may only worsen, and you may soon need cornea transplant surgery.
Causes
The exact causes of keratoconus are unknown, but genetic and environmental factors have been thought to play a role in developing the condition. One in ten people with this condition also has one or both parents with it. However, the risk factors that raise the chances of developing the condition besides a family history of keratoconus include rubbing the eyes vigorously and having certain conditions like hay fever, Ehlers-Danlos syndrome, asthma, and Down syndrome. Research also suggests that keratoconus may also be caused by the weakening of the corneal tissue, which may be caused by an imbalance of enzymes in the cornea. The development of keratoconus is also linked to exposure to UV rays of the sun, chronic eye irritation, and excessive rubbing.
Treatment
During the early stages, people with keratoconus may be able to correct their vision problems by wearing eyeglasses or contact lenses. However, if left much longer, the affected individual may have to use rigid, gas-permeable contact lenses or sometimes scleral lenses. Note that a cornea transplant may be required if the eye problem progresses to reach an advanced stage. Corneal collagen cross-linking is another treatment option that may help to slow down or even stop the progression of keratoconus, possibly eliminating the need to have a cornea transplant in the future. This treatment option may also be offered to complement the vision correction options mentioned above.
So, you need to understand that keratoconus is a progressive disease that affects the cornea and causes it to thin and bulge forward into a cone-like shape. Seeking treatment when the disease is in its early stages can help to slow or stop its progression. However, ignoring it may lead to invasive surgery, which could have been avoided. Note that family history of keratoconus is a major risk factor.
Featured